
Bedwetting is an issue that comes up in elementary school from time to time. Here are some resources to help support this situation for your students. The good news is that for many children the problem will resolve itself over time, or can be fixed through fairly simple treatment.
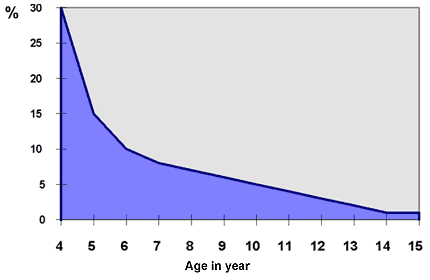
Bedwetting (also called nocturnal enuresis) is very common. As the following graph shows, almost a third of four-year-olds wet the bed. By the time they are 6, only one in 10 children wet the bed, and one in 20 by age 10. Bedwetting can sometimes continue into adolescence.
Percentage of children who wet the bed at different ages
Nighttime bedwetting. This type of bedwetting is a common sleep
a problem in children ages 6–12, occurring only during NREM sleep.
Primary enuresis (the child has never been persistently dry at night)
is associated with a family history of the problem, developmental lag,
or lower bladder capacity, and is unlikely to signal a serious
problem. Secondary enuresis (a recurrence of bedwetting after a year
or more of bladder control) is more likely to be associated with
emotional distress. Interventions include the use of reinforcement and
responsibility training (such as keeping a dry night chart), bladder
control training, conditioning (e.g., bedwetting alarms), and
sometimes medication. In the case of secondary enuresis, it might be
most helpful to determine any source of emotional stress and address
it directly. (For example, if a child starts wetting the bed at night
following parents’ separation or divorce, providing counseling to
address loss issues might help alleviate bedwetting.)When to see a doctor
You may wish to see a doctor about your child’s bedwetting if:
- your child is at least six years old (treatment for bedwetting is not recommended before this age as treatment is less effective and many children get better on their own)
- you or your child are troubled or frustrated by the bedwetting
- you punish, or are concerned that you might punish, your child for wetting the bed
- your child wets or has bowel movements in their pants during the daytime.
If your child has been dry at night for six months then begins to wet their bed again, it is important to see a doctor for evaluation.
The doctor will consider your child’s details and determine if there is a physical problem that needs to be addressed.
Source
BEDWETTINGNocturnal enuresis is the medical term for bedwetting. Most children
wet the bed occasionally or even nightly during the potty-training
years. In fact, it is estimated that seven million children in the
United States wet their beds on a regular basis. Controlling bladder
function during sleep is usually the last stage of potty-training. In
others words, it is normal for children to wet the bed while sleeping
during that learning process. Bedwetting is typically not even
considered to be a problem until after age 7.Bedwetting in children is often simply a result of immaturity. The age
at which children become able to control their bladders during sleep
is variable. Bladder control is a complex process that involves
coordinated action of the muscles, nerves, spinal cord and brain. In
this case, the problem will resolve in time. On the other hand, it may
be an indication of an underlying medical condition, such as
obstruction of the urinary tract. If bedwetting persists beyond the
age of 6 or 7, you should consult your pediatrician.There are both primary and secondary forms of bedwetting. With primary
bedwetting, the child has never had nighttime control over urination.
The secondary form is less common and refers to bedwetting that occurs
after the child has been dry during sleep for 6 or more months.
Secondary bedwetting may be caused by psychological stress but may be
the result of an underlying medical condition such as constipation or
urinary tract obstruction. With secondary bedwetting, contact your
doctor for an evaluation.Commonly prescribed behavioral methods for treating the problem include:
Establishing a regular bedtime routine that includes going to the bathroom
Waking your child during the night before he/she typically wets the
bed and taking him/her to the bathroom
Developing a reward system to encourage your child, such as stickers
for dry nights
Talking to your child about the advantages of potty-training, such as
not having to wear diapers and becoming a “big kid”
Limiting beverages in the evening – even those last minute water requests
Using a “bell-and-pad” which incorporates an alarm that goes off
whenever your child’s pajamas or bed become wet during an accident.
These systems teach your child to eventually wake up before the
bedwetting occursAs a last resort, a doctor may prescribe medication for bedwetting,
either for short or long-term use. Some examples are imipramine (an
antidepressant), which relaxes the bladder, and desmopressin, a
man-made copy of a normal body chemical that controls urine production
at night. Although medication usually helps, bedwetting typically
resumes once the child stops taking the medicine. As with any drug, it
is important to monitor your child’s response to the medication.Coping with Bedwetting:
There are products that parents can buy for school-aged children with enuresis:
Disposable absorbent underpants
Reusable absorbent underpants
Sleeping bag liners
Moisture alarms that go off when the child begins to wet the bedThere is no reason for punishment if your child wets the bed. Your
child cannot help it. Talk to your doctor about treatment options and
following these coping tips may help:Be patient, understanding and attentive
Do not talk about the bedwetting in front of others
Talk to your child about how the bladder works
Avoid fluids in the hours before bed
Links
